Oral melanoma in dogs is the most common oral tumor in the dog accounting for 30-40% of all canine oral tumors. Most patients are presented to their veterinarian for several reasons that can include: a mass seen in the mouth, dropping food, pain, foul breath, blood-tinged saliva, blood-stained toys or food, facial swelling and decrease in appetite/weight loss. If any of these signs or symptoms are seen, the first step is to bring your pet to your veterinarian for evaluation.
Breeds with a higher risk of developing oral tumors include the Cocker spaniel, German shepherd, German shorthaired pointer, Golden retriever, Gordon setter, Miniature poodle, Chow Chow and Boxer. Most melanomas are diagnosed in older dogs with the average age being 11 years of age.
Oral melanoma in dogs is an aggressive cancer that can metastasize (spread) in up to 80% of cases to the regional lymph nodes and lungs. These tumors are often pigmented, but there are some tumors that lack pigment (amelanotic). Due to the high metastatic potential, staging tests are recommended prior to definitive therapy since these tests can affect the patient’s outcome to treatment.

There are four different stages of oral melanoma in dogs. Dogs with stage I (or early stage oral melanoma in dogs) (<2 cm) and stage II (2-4 cm without lymph node or lung involvement) disease have a better long-term prognosis than dogs with stage III (4 cm or greater and/or lymph node metastasis) or stage IV (distant metastasis). The information below is broken into various categories to help you better understand the staging process, prognosis, and treatment for patients with oral melanoma.
Diagnosis/Staging
A biopsy is recommended for any abnormal mass in the mouth to obtain a definitive diagnosis.
-
Some melanomas can be difficult to diagnose, and additional testing (known as special stains) may be necessary if the biopsy is inconclusive. These stains are performed on the original biopsy sample that was submitted to the laboratory and may take about two weeks for the final results.
Prior to beginning any treatment, staging is recommended.
-
This includes chest radiographs or CT scan of the chest (to look for evidence of lung metastasis), full blood work (CBC and chemistry panel, urinalysis), and aspiration of the regional lymph nodes +/-CT/MRI to assess the extent of the tumor. Other tests may be advised depending on the health of the patient.
Prognostic Factors
Size of the tumor
-
<2 cm has a better prognosis than larger tumors.
Location
-
Animals with rostral tumors (towards the front of the mouth) have a more favorable prognosis.
-
Animals with oral tumors in the middle or back of the mouth tend to have a poorer prognosis, which may be related to the difficulty in surgical removal.
-
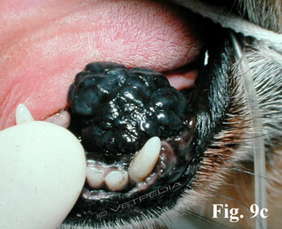
Melanomas on the lip tend to have a more favorable prognosis compared to ones located on the gingival/oral mucosa. Oral malignant melanoma in a dog. Photo courtesy of VetPedia
Stage
-
Stage I: median survival time is 12-18 months
-
Stage II: median survival time of 5-8 months
-
Stage III: median survival time of 3 months
Treatment for Oral Melanoma in Dogs
Treatment is divided into two sections: local control of the original tumor and systemic treatment due to the high potential for metastasis (spread to other sites).
Localized treatment
Surgery:
The treatment of choice for local control is surgery since this is the best chance to remove the entire tumor. Some patients may need a CT scan performed prior to surgery to determine the extent of disease and to ensure that surgery is the most appropriate local treatment. The goal of surgery is to remove all of the mass with adequate margins and this may involve removing a portion of the bone of the upper or lower jaw. Fortunately, most dogs do very well with this surgery and their quality of life is not affected.
Radiation Therapy:
Two forms:
-
Definitive therapy which is used in conjunction with surgery when the oral tumor is incompletely or narrowly excised in order to address the concern for tumor recurrence. Definitive therapy includes once or twice weekly treatments for 4-6 treatments. The goal of the radiation therapy is to help kill any residual disease that remains after surgery and decrease/slow the risk for recurrence.
-
Palliative therapy is performed when surgery is not an option or owners are not interested in aggressive surgery/treatment, but want to make their dog more comfortable. This involves once weekly treatments for 3-5 weeks in a row and there is minimal negative impact on the patient with this protocol. Fortunately, most melanomas are responsive to radiation therapy with 75% of patients experiencing a decrease in tumor size which can last 4-8 months depending on the stage of disease.
Systemic Therapy for Oral Melanoma in Dogs
Due to the high metastatic nature of these tumors, systemic therapy is also advised in addition to local therapy. Unfortunately, even when these tumors are controlled locally with surgery and/or radiation, most patients succumb to the disease because of metastasis to the lymph nodes and lungs as well as other organs. As a result, we encourage the use of the melanoma vaccine to try to combat the metastatic disease.

Canine melanoma vaccine (Oncept) is a xenogenic vaccine that is administered once every two weeks in the muscle of the inner thigh for 4 treatments. After the initial 4 doses, a booster vaccine is given once every 6 months thereafter. The vaccine is designed to stimulate the patient’s immune system to specifically target the melanoma cells. This vaccine is not known to have any systemic side effects, but rarely can cause some irritation at the injection site, a low-grade fever and depigmentation of fur or skin. The downside to the vaccine is that it can take a minimum of 2-3 months before the body’s immune system is stimulated enough to start targeting the melanoma cells for destruction.
-
This treatment can be used in combination with any of the local therapies listed above.
-
Chemotherapy is not commonly recommended because of the lack of efficacy. Chemotherapy has only been shown to be of benefit in less than 30% of patients and is usually reserved for patients with aggressive or fast-growing tumors in an attempt to slow them down in order to give the vaccine a chance to work.
-
Piroxicam is an oral non-steroidal anti-inflammatory medication that can help to stimulate the immune system. This is a non-steroidal anti-inflammatory that has been shown to have some activity against tumors by stimulating the immune system to attack cancer cells. This medication is administered at home on a daily basis. Side effects are uncommon, but can include vomiting, diarrhea, anorexia, and gastrointestinal ulcers. For most patients, these side effects may be avoided by giving the medication with food. Rare toxicity of the liver and kidneys can be noted, so periodic blood work is recommended to monitor for any adverse effects. Unfortunately, only 10-20% of patients will experience a benefit with piroxicam.
GOAL
The ultimate goal of any treatment is to improve your pet’s quality of life and your veterinary oncologist will work with you to determine the treatment option that you feel most comfortable with.
